In a 2003 speech, John Kerry complained about the Bush administration, saying:
Nothing illustrates this administration’s anti-science attitude better than George Bush’s cynical decision to limit research on embryonic stem cells.
During the heat of the “stem cell wars,” this was a common refrain. Life-saving treatments could be produced with embryonic stem cells, and anyone who questioned whether or not it was morally acceptable to destroy one life in order to experiment with saving another was “anti-science.” Never mind that there are stem cells in everyone’s body, commonly called adult stem cells, and those stem cells also have the potential to cure illnesses. Everyone “knew” that using embryonic stem cells would be better.
What’s the difference between embryonic stem cells and adult stems cells? Well, most of the cells in your body have specific tasks. Your skin cells perform one set of tasks, while your muscle cells perform another set of tasks, your liver cells another set of tasks, etc., etc. These cells have all “specialized” so they can perform their tasks efficiently. A stem cell, by contrast, is a cell that hasn’t yet “specialized.” It can develop into many different cells, depending on your body’s needs.
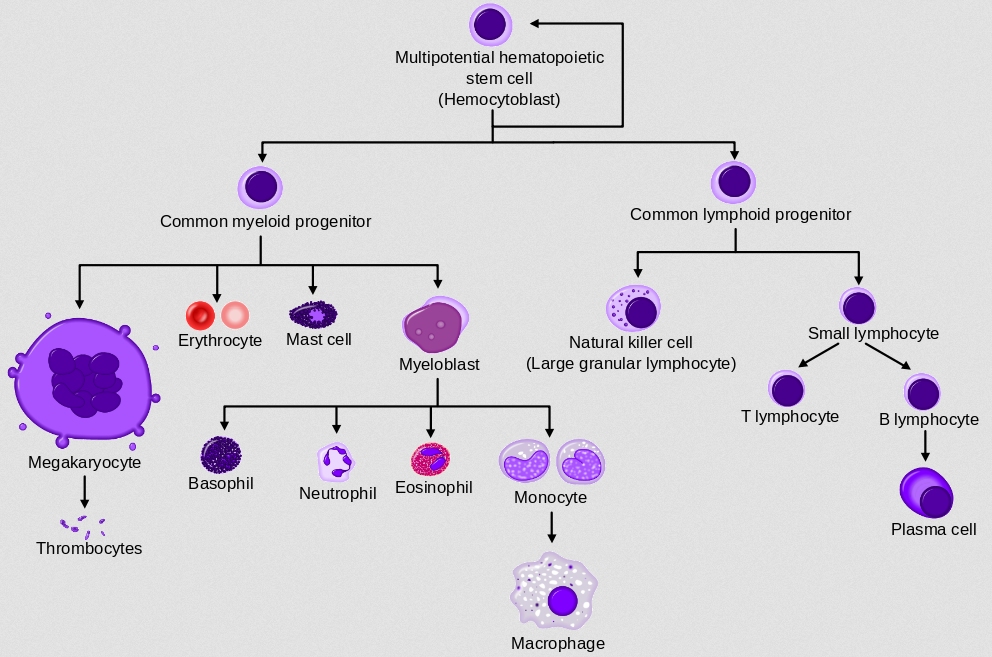
Embryonic stem cells end up developing into all the cells that make up the body, so they are thought to be very, very flexible when it comes to what they can develop into. However, to get those stem cells, you have to kill the embryo. Adult stem cells, on the other hand have already specialized to some degree. For example, the drawing at the top of this post shows how an adult stem cell found in bone marrow can develop into various different blood cells. While that shows some serious flexibility, bone marrow stem cells don’t normally develop into wildly different cells, like skin cells. As a result, it is thought that adult stem cells aren’t as flexible as embryonic stem cells. On the positive side, however, you don’t have to kill anything to get adult stem cells.
The scientific question, then, boils down to this: “Is it worth working with stem cells that might not be as flexible as embryonic stem cells in order to avoid killing human embryos?” Those who answered that question with a “yes” have been routinely labelled “anti-science.” However, now that we are 13 years past Mr. Kerry’s speech, we can see that adult stem cells have, in fact, demonstrated success in treating a wide variety of illnesses. Obviously, a lot more research has to be done, and none of these treatments are standard or routine yet. Nevertheless, it is now clear that if there is a limit to the abilities of adult stem cells when it comes to treating illnesses, we haven’t reached it yet.
That brings me to the reason I am writing this article. Over the past few days, I have seen two more examples of adult stem cells successfully treating illnesses. The first example appears in JAMA Neurology, a specialized publication of the Journal of the American Medical Association. This study dealt with the treatment of myasthenia gravis, a degenerative neuromuscular disorder that can be life-threatening. The authors of the study followed 7 patients that were treated with stem cells from their own bone marrow, and all of them achieved stable remission and were freed from ongoing myasthenia gravis therapy!1
Now, of course, this is a small study, and while some patients were followed for 13 years, others were followed for only 2.5 years. In addition, the authors note that specialized patient care is necessary for this treatment to be effective. As a result, they only recommend it for institutions that have experience treating patients with myasthenia gravis. Nevertheless, it at least shows the potential of using a patient’s own adult stem cells to treat a neuromuscular disorder.
The other study isn’t as groundbreaking, but it does provide new insights into the use of adult stem cells to treat heart failure. The authors reported on a randomized, double-blind, placebo-controlled study of end-stage patients with serious heart failure. The only hope such patients have is for a heart transplant. Since that wasn’t possible for these patients, they agreed to be part of a study that examined the efficacy of treating their heart failure with (once again) stem cells from their own bone marrow. The procedure typically took only two hours, and most patients were released from the hospital the day after the procedure was done.
After 12 months, those who received the treatment were 37% less likely to have been taken to a hospital and 50% less likely to die than those who received a placebo.2 While those numbers aren’t as wonderful as the numbers in the myasthenia gravis study, they are significant. In addition, the study was the largest ever done on this kind of treatment. Thus, it clearly shows that patients who need a heart transplant have at least one other option, thanks to adult stem cells.
Far from being anti-science, then, caution about using embryonic stem cells is scientifically reasonable. Adult stem cells have shown quite a lot of promise, and they avoid the moral problems associated with killing embryos.
REFERENCES
1. Adam Bryant, et. al., “Myasthenia Gravis Treated With Autologous Hematopoietic Stem Cell Transplantation,” JAMA Neurology, 2016, doi:10.1001/jamaneurol.2016.0113
Return to Text
2. Dr. Amit N Patel, et. al., “Ixmyelocel-T for patients with ischaemic heart failure: a prospective randomised double-blind trial,” The Lancet, 2016, doi:10.1016/S0140-6736(16)30137-4
Return to Text

God has given man so many ways to treat himself, and yet man still seems infatuated with destroying himself. God help us.
Appreciate your thoughts on this topic. My wife is legally blind (optic nerve hypoplasia). I am always on the lookout for new research that may one day treat her. There is an interesting unorthodox clinical trial in Flordia (mdstemcells) (patient funded), where stem cells are taken from your bone marrow and injected for treating / curing ophthalmic disease. Very little results have been published, and I doubt anything will be until next year. I always hopeful that this research will eventually bring ways to cure the current incurable.
‘This time you are to imagine yourself to be a surgeon, a truly great surgeon. Among other things you do, you transplant organs, and you are such a great surgeon that the or- gans you transplant always take. At the moment you have five patients who need organs. Two need one lung each, two need a kidney each, and the fifth needs a heart. If they do not get those organs today, they will all die; if you find organs for them today, you can transplant the organs and they will all live. But where to find the lungs, the kidneys, and the heart? The time is almost up when a report is brought to you that a young man who has just come into your clinic for his yearly check-up has exactly the right blood-type, and is in excellent health. Lo, you have a possible donor. All you need do is cut him up and distribute his parts among the five who need them. You ask, but he says, “Sorry. I deeply sympathize, but no.” Would it be morally permissible for you to operate anyway? Everybody to whom I have put this second hypothetical case says, No, it would not be morally permissible for you to proceed.’
–Judith Jarvis Thomson
This second hypothetical followed the one where a trolley driver has to choose between saving 5 lives or one life by deciding who he must hit. Everyone says it is okay to turn the trolley to hit one person rather than hitting the five people. While the two hypotheticals are interesting, they aren’t exactly parallel, are they? In the first, the trolley driver MUST kill either the one or the five. In the second, the surgeon doesn’t kill anyone by doing nothing. He or she just lets nature take its course.
Yes, but the trolley isn’t the parallel here. Basically everyone acknowledges it would be evil to kill someone for parts, and yet people are attacked for objecting to literally that in the case of embryos.
(That Thomson brought the hypothetical into common consideration is a little ironic.)
To kill a human being is murder if its intentional. Killing a human being otherwise is not intentional but still sending someone to their eternal destiny.
since conception is where the soul comes into the body and it never goes some other time then aby interference is killing a human being.
Its not relevant if it helps someone. Nobody argues people should be killed for their organs to be used to help others.
My sister-in-law just discovered a stem-cell therapy that is gaining in popularity when she wa doing research about having total knee replacement surgery. There are clinics that are harvesting the patient’s stem cells and injecting them into the knee joint. Apparently the orignial thought was that the stem cells would regrow missing cartilage. This doesn’t happen but up to 70% of patients have relief of their knee pain and improvement in joint function. There are, of course, ongoing trials; they aren’t sure how long the effect lasts (If I remember correctly the longest so far has been 2 to 3 years) but replacing surgery with its possible complications and long rehab period for a therapy with just a couple of needle sticks sounds pretty good to me.
My sister-in-law decided that the odds were good enough for her and she’s going to have this done rather than surgery. I’m interested to see what kind of results she gets.