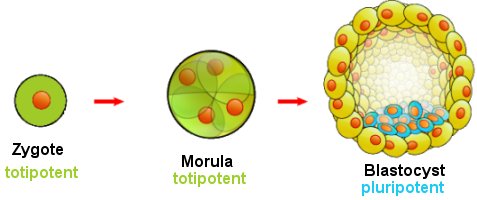
When your mother’s egg cell was fertilized by your father’s sperm cell, the result was a single cell, called a zygote. That cell had all the information necessary to develop into the person you are today. In other words, it could produce everything necessary to build you. So that single cell had the capability of developing into any human cell. We call such cells totipotent cells. Of course, in order to make all those cells, the zygote had to start reproducing, resulting in an embryo.
As this cell (and its progeny) reproduced, the number of cells in the embryo grew. When that reproduction had produced about 12 cells, you were in the morula stage of your development, and on a microscopic level, you resembled a mulberry. As your cells continued to reproduce, they formed a hollow sphere called a blastocyst. At one end of the hollow sphere, there was a bunch of cells called the inner cell mass, which is represented by the blue cells in the illustration above. That inner cell mass developed into all the organs and tissues that make up your body.1
Interestingly enough, however, the cells in that inner cell mass were no longer totipotent. They could not, for example, form the kind of cells that make up the outer layer of the blastocyst, which are shown in yellow in the illustration above. However, they could end up becoming any of the cells in any of the organs or tissues of your body. As a result, they are called pluripotent cells. As they continued to reproduce, they started “choosing” what kind of cell they would become. Some of those pluripotent cells, for example, became skin cells. Once they did that, we say that the cells had differentiated. This means they lost their pluripotency, and would no longer be able to become some other type of cell. As a result, they would end up doing the same job for the rest of their lives.
Pluripotent cells are often called stem cells, and they have a lot of potential in medicine. After all, if someone suffers from severe organ damage, I could theoretically get his or her body to rebuild that damaged organ if I supplied it with enough stem cells. The stem cells could then differentiate into whatever cells are needed to replace those that died when the organ was damaged. While this sounds wonderful, there is a problem. The most ready source of pluripotent cells come from the blastocyst stage of an embryo’s development. If I remove those pluripotent cells from the blastocyst, I have embryonic stem cells, but unfortunately, the embryo dies.
Are embryos the only source of pluripotent stem cells? No. There are adult stem cells that can be found in any fully-developed person, but there is a problem with them as well. It is hard to find pluripotent adult stem cells. Most adult stem cells have partially differentiated, so the kinds of cells they can develop into are limited. For example, you have adult stem cells in your bone marrow. They can develop into any type of blood cell (red blood cell, macrophage, neutrophil, etc.), but they cannot develop into skin cells, nerve cells, muscle cells, etc. As a result, we call them multipotent. They still have choices as to what kind of cell they can become, but those choices are restricted compared to those of a pluripotent cell.
So if you want pluripotent stem cells, embryos are the easiest way to get them. Of course, it is also the unethical way to get them, because you end up killing a human being. So people who are concerned about ethics have been trying to find another way to get pluripotent stem cells. Back in 2007, three separate research groups found a way to take an adult skin cell and reprogram it to become pluripotent again.2 While those three groups (and others) have shown that such cells, called induced pluripotent stem cells, can develop into many different types of cells, one important question remains: Are they truly as pluripotent as embryonic stem cells?
Well, we are one step closer to answering this question, thanks to researchers at the University of Wisconsin-Madison. In a study published online September 11, they compared four embryonic stem cells to four induced pluripotent stem cells. Specifically, they compared the proteins that the cells produced. After all, a skin cell produces a set of proteins that is quite distinct from a muscle cell, so the set of proteins that a cell makes is a good probe of what the cell can actually do.
What was the result? They found that the embryonic stem cells and the induced pluripotent stem cells are at least 99% the same when it comes to the proteins they produce!3 In fact, in some measurements, they found that one embryonic stem cell produced proteins that were more similar to one of the induced pluripotent stem cells than another embryonic stem cell. As a result, it seems that from a protein standpoint, there is very little difference between embryonic stem cells and induced pluripotent stem cells.
This is great news for those of us who want to see the medical advances that pluripotent stem cells can produce without the murder that accompanies embryonic stem cell use!
REFERENCES
1. Rod R. Seely, Trent D. Stephens, and Philip Tate, Anatomy and Physiology, Fifth Edition, 2000, pp. 962-963
Return to Text
2. Cyranoski D, “Simple switch turns cells embryonic”. Nature 447: 618–619, 2007.
Return to Text
3. Douglas H Phanstiel, et. al., “Proteomic and phosphoproteomic comparison of human ES and iPS cells”. Nature doi:10.1038/nmeth.1699, 2011.
Return to Text

Two things:
1. So are you telling me that story my parents told me about an alien ship delivering me to them isn’t true?
2. How does this effect Peyton Manning’s ability to return this season and save the Colts from Old Man Collins?
Black Sheep, I love it when you comment!
1. Of course the aliens ship story isn’t true. A stork brought you to them!
2. If Peyton Manning returns, he won’t save the Colts unless the defense steps up.
I wonder how long it will take for supporters of embryonic stem cell research to admit that a superior method has been discovered, making theirs obsolete. Maybe as soon as they can get new grant proposals written? 🙂
As an aside, I saw this article at The Scientist: http://the-scientist.com/2011/09/14/skipping-pluripotency/ It appears they are trying to convert cells directly from one type to another, skipping the induced pluripotent step altogether. Fascinating stuff!
Thanks for the link, Shevrae. I had not seen that.
This is good news and just another example of why researchers must be guided by proper moral principles if they are to avoid harming human life but rather promote its preservation.
I read recently that Mississippi has a ballot initiative that specifies that personhood begins with conception. If passed, this would provide a direct legal challenge to the evil Supreme Court decision that legalized abortion by skirting the question of when legal personhood begins.
Many people (including some Christians) seem confused about when human life begins, but as you clearly point out, the science behind this question is not confusing at all.
David, you are most certainly correct that from a scientific standpoint, there is no question about when human life begins. Once the sperm fertilizes the egg, you have a new genome that defines a new human life!
Dr. Wile, I’m glad you like my comments. I always try to comment when I can actually make sense out of you’re trying to say!
1. Wow! A stork!?! Glad the bird flu wasn’t around when I was delivered!
2. Seriously!!! Of course, the offensive line could also help Collins out a bit more. Last year half our offense was out and we still managed to be respectable. Now we have one guy out and suddenly no one can make play!!! GRRRRR!
Black Sheep, you are now starting to understand what it was like being a Colts fan from 1985 to 1999!
This was a cool post. IPSCs have interested me ever since I wrote a 7 page paper on them in freshman year of college and then had to present to the class about them.So it was nice to seem an update. 🙂
I am glad it was helpful, Vivielle!
That was great! From time to time, I find myself in discussions about the “when does life begin” question. It’s pretty simple — the sperm is ‘living’, the ovum is ‘living’ and a new *human* life is created when they fuse together to produce a new human genome, just like you said. Appreciate you Dr. Wile, and your unequivocal exposition of the science here.
Thank you so much, Elizabeth. In a previous post, I quoted Dr. Jermoe L. LeJeune, the brilliant geneticist who was the first to demonstrate a link between certain diseases and chromosomal abnormalities. He says it all:
Thanks for the link… incredible research! I’ll definitely be hanging onto that for future reference.